Beyond "Normal": Why Your Labs Might Be Missing the Big Picture in Perimenopause
- Apr 2
- 6 min read
I talk to women every week in their 40s and 50s who are noticing weight gain, their sleep is trash, they can’t concentrate, no energy, moody, zero sex drive, and feeling like they're in a body that isn't their own. To make matters worse, they go to their doctor and it’s brushed off as normal aging. Sometimes they’ll tell you to relax and strap in for the ride, and sometimes they’ll offer you an antidepressant. I have heard some WILD stories but that's not what this is about today..
A lot of these simple symptoms are common, but that doesn’t mean you have to deal with them for years on end with no relief in sight.
I want to talk about the labs I’d want you paying attention to if you were a client of mine. But first let’s touch on what’s considered “normal” on your labs.
Why “normal” labs can still miss the bigger picture
When you go to your doctor and they pull your labs, you’ll get results back with a range of what’s “normal”. Most standard lab ranges are built to identify disease, not to help you feel your best. They are based on broad reference intervals from the general population. That means you can fall inside the lab’s normal range and still be far from optimal.
Let me be clear…this is not a knock on your doctor. Most physicians have limited time, are trained to rule out disease first, and work inside a system built for diagnosis and treatment. Perimenopause is not a “disease”. It’s a normal part of aging. So to them, there is nothing “wrong” but herein lies the problem because you don’t feel like nothing’s wrong.
Our traditional healthcare model is not designed to help women thrive through this stage of life.
Functional Ranges
Functional ranges are tighter. They give us a better lens for prevention, early pattern recognition, and quality of life. With functional ranges we don’t wait for disease, we get curious and we use this data alongside of your lifestyle and how you feel (CRAZY idea huh?) to think critically about getting you to a better place.
What’s happening in this stage?
Late perimenopause and menopause can shift a lot at once:
Blood sugar regulation
Cholesterol patterns
Inflammation
Thyroid function
Recovery and sleep
Sex hormone production and signaling
This is one reason women can feel off long before anything is flagged as a diagnosable problem-and it all reality, it won’t be in our traditional healthcare system.
So let’s get to it, and before I do, I want to say this really important caveat:
Lab interpretation is VERY MUCH an art and a science.
The lens through which you view the labs, the context of the person’s lifestyle, and how much data you have matter an incredible amount. It’s not unheard of for me to spend hours interpreting labs in the context of my client’s situation. Almost every aspect of your lifestyle matters when it comes to looking at and interpreting your labs in a way that you can actually learn something and take action from.
So, labs on their own…won’t tell you much. You have to know how to interpret the data and then what to do with it.
That being said, I know I can’t help everyone, so here are the labs I pay closest attention to so you can take an active role in managing your own health because in the end, that’s what it’s truly about!
Here are the labs I pay closest attention to:
1. Fasting insulin, fasting glucose, and A1C
These three tell a much better story together than any one marker alone. A1C may still look fine while fasting insulin is already climbing. That matters. Insulin often rises before glucose and A1C become obviously abnormal, which can be an early warning sign that your metabolism is under more strain than you realize. This is super common in perimenopause and menopause and can make weight gain easier and weight loss more challenging.
Ranges to know:
In this stage of life, these markers matter because estrogen shifts, poor sleep, stress, lower muscle mass, and less movement overall can all make blood sugar regulation worse.
2. Triglycerides, HDL, and LDL
Lipids often change in perimenopause and menopause, especially as estrogen declines. LDL often rises in this stage and deserves context, not panic. I do not look at LDL in isolation. I want to see it alongside triglycerides, HDL, inflammation, insulin, A1C, thyroid markers, and the full clinical picture.
Ranges to know:
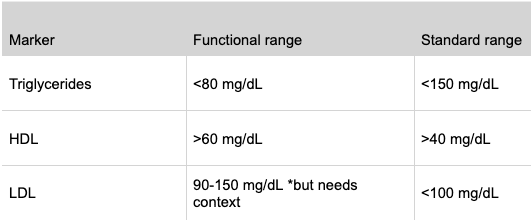
If triglycerides are high and HDL is low, that often tells me more about metabolic stress than LDL alone.
3. Vitamin D and hs-CRP
These are two simple but important markers. Vitamin D plays a role in immune function, mood, bone health, and overall resilience. hs-CRP gives us a window into low-grade inflammation, nondescript inflammation. Elevated CRP also correlates to a higher risk of a cardiac event. This is also a reminder that heart disease is the number one killer of women in the US.
Ranges to know:

When you are dealing with fatigue, aches, poor recovery, or just feeling inflamed and puffy, these are worth paying attention to and often not check on standard labs.
4. Thyroid markers
When you tell your doctor you want your thyroid checked, they’ll likely only pull your TSH. A “normal” TSH does not always mean thyroid function is optimal. I always look at TSH with free T3 and free T4 for a more complete picture. In perimenopause, thyroid symptoms can overlap heavily with hormone symptoms, which is one reason women get dismissed or confused. Ranges to know:
If a woman is tired, cold, foggy, gaining weight easily, or struggling with hair loss and mood changes, I want to see more than a single thyroid number.
Ranges to know:

5. Ferritin and iron markers
Ferritin can be especially important in women moving through late perimenopause, especially if there has been a history of heavy or irregular bleeding earlier in the transition. At the same time, ferritin is also an acute phase reactant, which means inflammation can push it up even if iron storage is not high. This is why context matters.
Ranges to know:

Low energy, poor recovery, hair changes, and reduced exercise tolerance can all overlap here. Iron levels in the body can be high or low during this time and just pulling the serum iron does NOT tell you the iron levels in the body.
6. Sex hormones including testosterone
This is the part of the conversation where nuance really matters. Hormones like estradiol, progesterone, testosterone, FSH, and LH can give us useful information. But in perimenopause, they can also be one of the easiest places to get confused because hormones are not static.
In late perimenopause, estrogen can swing high and low. Progesterone often starts dropping earlier and more consistently as ovulation becomes less predictable. Testosterone will decline over time as well, which can affect energy, strength, recovery, mood, and libido.
FSH and LH will rise as the brain and ovaries have to work harder to communicate, but those numbers can still bounce around depending on the stage of transition.
This is why one hormone panel does not always give a clear answer and why symptoms and context matter.
Hormones are influenced by:
Where you are in your cycle
Whether you are still ovulating regularly
Whether you are in late perimenopause or fully menopausal
Whether you are using hormonal birth control or hormone therapy
Stress, sleep, under-eating, and overall metabolic health
You can have symptoms that clearly point to hormonal shifts, but your labs may not tell the full story in one single lab draw. That does not mean testing is useless. It just means your labs should be interpreted alongside your symptoms, cycle patterns, age, and the rest of the lab picture.
In this stage of life, I care less about chasing one “perfect” hormone number (it doesn’t exist!) and more about understanding the overall trend:
Are hormones fluctuating in a way that matches what you are feeling?
Is ovulation likely becoming less consistent?
Are symptoms pointing to lower estrogen, lower progesterone, lower testosterone, or a mix?
Are blood sugar, inflammation, thyroid, and stress also contributing?
That bigger-picture approach is always more helpful than obsessing over one isolated hormone result.
Labs are data, not the whole story Labs matter.
Symptoms matter. Your cycle history matters. Sleep, stress, muscle mass, nutrition, and activity matter too.
This is why I do not believe in looking at one isolated number and making sweeping conclusions. The goal is not to obsess over every marker. The goal is to understand the bigger picture and identify the biggest needle movers.
My final thoughts…
If you have been told everything looks normal, but you do not feel like yourself, it may be time to look closer. Not from a place of fear. From a place of education and context. The right labs, interpreted well, can help you understand what is changing, what deserves attention, and what appropriate support or treatment options may be worth discussing.
Want help making sense of your labs?
If you want support looking at your labs through the lens of perimenopause, metabolism, lifestyle, and the bigger picture, apply for coaching. This is one tool I use to assess your lifestyle and get you on the path to feeling your absolute best! Through coaching, we connect the dots and build a plan around your lifestyle, goals, and preferences, and not just your lab report.
Disclaimer: This content is for educational purposes only and is not intended to diagnose, treat, or replace medical care. Lab interpretation should always be done in context and in partnership with your physician or qualified healthcare provider.



Comments